by Alan Jordan
Patients are often confused or disappointed when they are told that they are experiencing “non-specific” lower back pain because they understandably do not know what it means. In fairness, it is a generic diagnosis which means;
- Their condition is not serious
- We are confident that their pain is not caused by an inflammatory condition, a tumour or otherwise
- We are not – nor can we be – exactly certain as to what tissues are causing their pain.
How can this be?
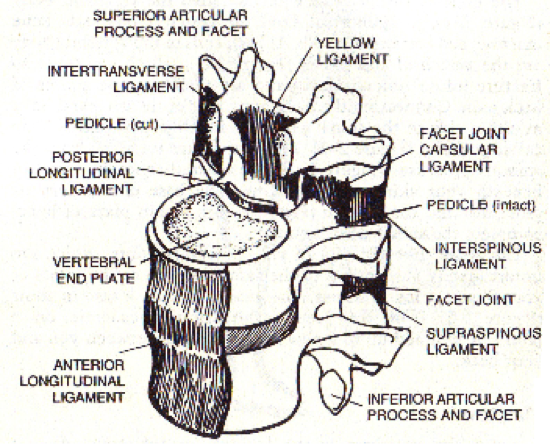
The illustration below shows just how complex a structure the spine and its individual segments are.
Each and every one of these differing tissues can result and/or contribute towards pain.
Most back injuries will involve several tissues being injured and it is therefore impossible for clinicians to provide a pure and proper diagnosis as the pain experienced by the patient will not distinguish between the differing tissues. For example, joint pain will feel like disc pain and so forth. Once again, injured joints will impact the muscles and joint capsules which will then result in a mixture of pain which neither the clinicians or the patient can accurately classify. Therefore, the term “non-specific” lower back pain.
To add to the confusion
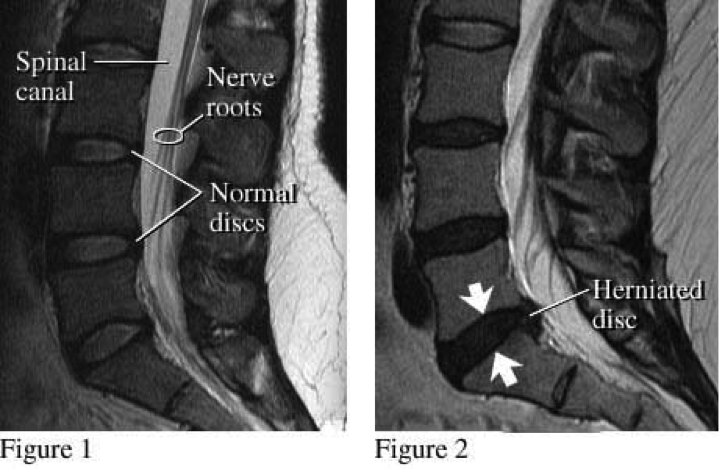
Even with a thorough case history and physical examination + MRI scans we are not always able to identify the source of pain. Below are MRI scans of the lower back.
Figure one illustrates a healthy spine with well-defined discs which are adequately filled with fluid and all disc heights are well maintained. Figure two illustrates a disc herniation which is clearly visible as is the fact that the lower discs no longer have any fluid in them.
Clear Enough?
One would naturally think that the patient scans of Figure 2 – which are clear enough – would lead one to believe that this patient has a disc herniation and is likely in need of surgery. Even this is not a certainty and many patients will MRI scans similar to Figure 2 are not experiencing any pain at all.
These are termed “silent” disc herniations.
Working Diagnosis
The vast majority of patients – at least from honest clinicians – will be told that they have non-specific lower back pain because we cannot provide them with an anatomically secure diagnosis which identifies the precise tissue that is causing the pain. We then work with a “working diagnosis” and initiate treatment while monitoring regularly monitoring results their symptoms.
If progress is unsatisfactory we can request further investigations or refer to another clinician.
Conclusion
This article has attempted to explain why diagnosing lower back pain is not as straight forward as one might think. We are fortunate that at our clinic we have a very broad array of clinicians who work in a cohesive manner – and we often seek advice from our colleagues.